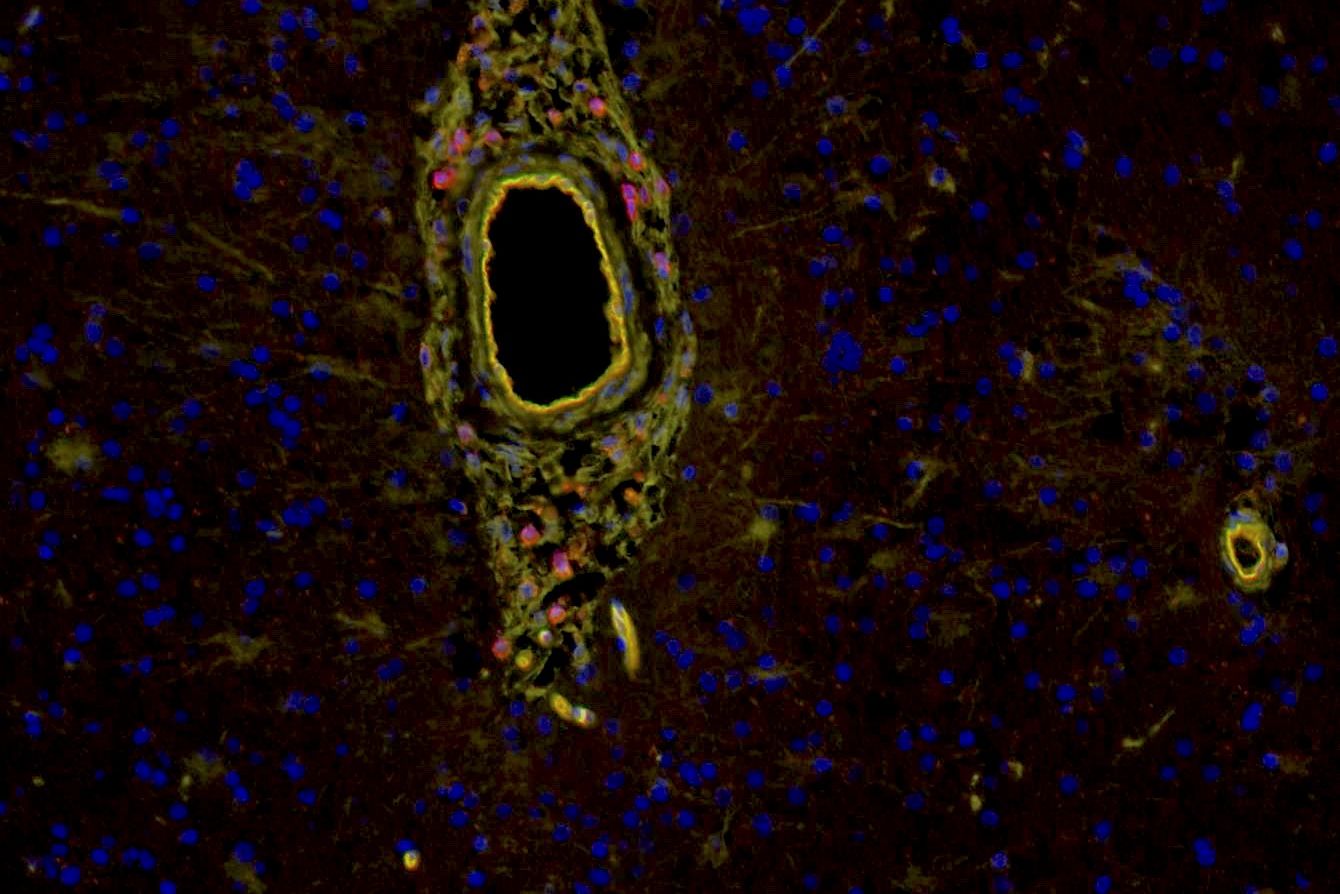
(Vienna, 28 August 2018) Glioblastoma is a brain cancer with devastating prognosis. A new collaborative study by scientists from CeMM, MedUni Vienna and the Austrian Brain Tumor Registry network demonstrates how epigenetic analysis of tumor samples collected in routine clinical practice could be used to better classify and treat the disease. The results were published in Nature Medicine.
Glioblastoma is an aggressive brain cancer with a high degree of molecular heterogeneity among the cancer cells. This results in evolutionary selection for those cells that can withstand drug treatment. In order to develop better therapies for glioblastoma, detailed knowledge about the molecular heterogeneity of the tumor cells will be crucial, given that this heterogeneity provides the substrate from which drug resistance evolves.
Whether and how epigenetic regulation changes when a glioblastoma becomes therapy-resistant has been a largely unsolved question. To investigate the role of epigenetics in glioblastoma disease progression, the research group of Christoph Bock, Principal Investigator at the CeMM Research Center for Molecular Medicine of the Austrian Academy of Sciences, analyzed DNA methylation in more than 200 glioblastoma patients, focusing on the epigenetic changes that occur during glioblastoma disease progression.
In close collaboration with scientists at the Medical University of Vienna and clinicians at eight hospitals throughout Austria , a study published in Nature Medicine (DOI: 10.1038/s41591-018-0156-x) identified epigenetic changes that accompany glioblastoma progression and predict patient survival.
This research builds on the Austrian Brain Tumor Registry, spearheaded by Adelheid Woehrer from the Institute of Neurology at the Medical University of Vienna, who is a senior and corresponding author of the study. Combining epigenetic data with brain imaging and digital pathology, the study established important links between glioblastoma at the level of molecules, cells and organs. These associations can be exploited for improving disease classification. Moreover, this study provides a rich resource for understanding the role of epigenetics in glioblastoma and a new toolset with broad relevance for personalized medicine.
Publication
Klughammer J*, Kiesel B*, Roetzer T, Fortelny N, Kuchler A, Nenning KH, Furtner J, Sheffield NC, Datlinger P, Peter N, Nowosielski M, Augustin M, Mischkulnig M, Ströbel T, Alpar D, Erguener B, Senekowitsch M, Moser P, Freyschlag CF, Kerschbaumer J, Thomé C, Grams AE, Stockhammer G, Kitzwoegerer M, Oberndorfer S, Marhold F, Weis S, Trenkler J, Buchroithner J, Pichler J, Haybaeck J, Krassnig S, Mahdy Ali K, von Campe G, Payer F, Sherif C, Preiser J, Hauser T, Winkler PA, Kleindienst W, Würtz F, Brandner-Kokalj T, Stultschnig M, Schweiger S, Dieckmann K, Preusser M, Langs G, Baumann B, Knosp E, Widhalm G, Marosi C, Hainfellner JA, Woehrer A#, Bock C# (*These authors contributed equally to this work; #These authors jointly directed this work). The DNA methylation landscape of glioblastoma disease progression shows extensive heterogeneity in time and space. Nature Medicine, August 27, 2018. DOI: 10.1038/s41591-018-0156-x
Funding
The study was funded by the Austrian Science Fund, the European Union, the Austrian Academy of Sciences, and the European Research Council.